Kidney Cancer is not just one disease. There are a number of different cell types, each of which responds somewhat differently to treatment. Dr. W. Marston Linehan and his team at the U.S. National Cancer Institute has done extensive work in understanding the different kinds of kidney cancer.
 While clear cell renal cell carcinoma (ccRCC) is the most common type of kidney cancer, there are several other important cell types as well:
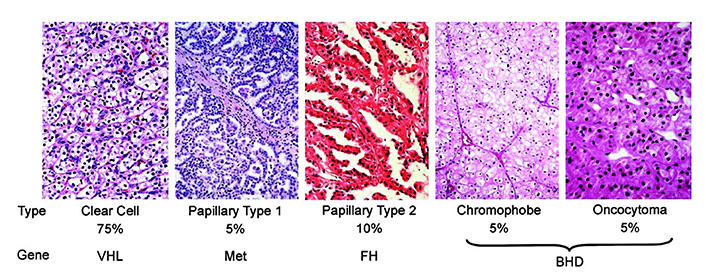
While clear cell renal cell carcinoma (ccRCC) is the most common type of kidney cancer, there are several other important cell types as well:
- Clear cell = 75%
- Papillary type I = 5%
- Papillary type II = 10%
- Chromophobe = 5%
- Oncocytoma = 5%
In each case, a different genetic alteration is present, which changes the chemical processing in the cell and makes it more or less responsive to the action of each of the drugs on the market. Thus the genetic analysis of the tumor tissue may be important in choosing the right drug.
In addition, if a “germline” mutation is present in every cell of this patient, there may be more than just kidney cancer to be concerned about. Approximately 5-10% of people with kidney cancer may have a hereditary condition, and the percentages are higher if the patient is younger than age 50. The tumor tissue type may be helpful in determining what genes should be screened for in genetic testing, and what other organ systems may be at risk for medical issues. If one of these syndromes is present, it will influence the optimal choice of treatment for this patient, and influence a plan of surveillance to watch for other issues.
- Clear cell — screen for changes in the VHL gene, implicated in von Hippel-Lindau (VHL)
- The most common type of kidney cancer is called clear cell renal cell carcinoma (RCC). This accounts for up to 80% of kidney cancer. It is more common in men than women and usually occurs after age 55. Clear cell RCC is thought to arise from the cells that line the kidney tubules where urine is made. Through a microscope, the cells look clear and pale. This type of kidney cancer is usually due to a mutation in the von Hippel Lindau (VHL) gene. There are families with inherited mutations of VHL who develop kidney cancers in addition to other medical problems (see VHL Syndrome below). The majority of people, however, who develop clear cell RCC have a non-inherited or “sporadic” version. As a result of the medical research that has found this gene abnormality, there have been great advances in the treatment of this type of kidney cancer.
- Suggested Resources - http://www.kidneycancer.org/ and http://ikcc.org/
- Papillary — The second most common type is called papillary renal cell carcinoma (RCC). Papillary rcc accounts for about 15% of kidney cancers. The name is from microscopic finger-like projections (called papillae) in some, if not most, of the tumours. There are 2 main types of papillary kidney cancer:
- Papillary type 1 — screen for changes in the MET proto-oncogene, implicated in Hepatocellular Carcinoma (HCC) and Hereditary Papillary Renal cell carcinoma (HPRCC).
- Type 1 is generally less aggressive. There is a small subset of people who can inherit this type of papillary renal cell carcinoma. Papillary type I RCC, in both the sporadic and hereditary forms, is associated with a mutation of the MET oncogene. An oncogene is a gene in cells that promotes growth and this cancer is associated with abnormalities of the MET gene.
- Papillary type 2 — screen for changes in the FH gene, implicated in Hereditary Leiomyomatosis and Renal Cell Cancer (HLRCC)
- Type 2 tends to be more aggressive, and in rare cases is part of a hereditary syndrome as well. Papillary type 2 tumors occur both sporadically and in patients who have the familial syndrome of hereditary leiomyomatosis and renal cell carcinoma (HLRCC). The genetic mutation associated with HLRCC is in the gene known as fumarate hydratase (FH).
- Suggested Resources - www.hlrccinfo.org and http://www.cancer.net/cancer-types/hereditary-papillary-renal-cell-carcinoma
- According to this source, these statistics seem to be stage dependent. "Type I appears to be more common than type II in general but in a study of patients being treated for metastatic RCC, Upton 2003 found 14 type II patients and only 2 type I patients. This remarkable reversal of the prevalence of type I and type II strongly suggests that type II metastasizes much more commonly than type I."
- Papillary type 1 — screen for changes in the MET proto-oncogene, implicated in Hepatocellular Carcinoma (HCC) and Hereditary Papillary Renal cell carcinoma (HPRCC).
- Chromophobe — screen for changes in the FLCN gene, implicated in Birt-Hogg-Dubé syndrome (BHD).
- This accounts for about 5% of RCC. Overall this is usually less aggressive than clear cell RCC and is usually confined to the kidney. However there are times it can be more serious and can spread.
- Oncocytoma — screen for changes in the FLCN gene, implicated in Birt-Hogg-Dubé syndrome (BHD).
-
This accounts for about 5% of renal tumours. An oncocytoma is usually a solitary tumour that is benign. It is often diagnosed on biopsy or pathologically after treatment of presumed RCC . However, a form of oncocytic cancer, chromophobe RCC, can occur.
-
Suggested Resources - http://www.oncocytoma.info
-
- Rarer Types
-
Collecting Duct renal cell carcinoma (Bellini duct carcinoma) - This subtype is very rare. The major feature is that the cancer cells can form irregular tubes and starts in a different part of the kidney tubule. This tumour type is very aggressive, and has traditionally been treated with chemotherapy although the best treatment is not yet known.
-
Genetic Translocation Cancer - This is a distinct form of kidney cancer that can occur in young adults (especially females) and probably children. It may make up approximately one-third of pediatric RCC. This can be diagnosed by special staining (immunohistochemical staining) of tissue from the kidney tumour. There are genetic abnormalities called translocations in the TFE3 gene (Xp11.2 translocation).
Approximately 10% to 15% of translocation RCCs occur in children who had prior chemotherapy for a prior cancer. Therefore translocation RCCs should be added to the list of chemotherapy-associated secondary cancers in children.
-
Renal medullary cancer - This rare yet aggressive cancer can be found in young adults that have sickle cell trait or rarely sickle cell disease, an inherited disease related to their haemoglobin in their red blood cells. In those with sickle cell trait the person carries one normal copy of the hemoglobin A gene (HbA) and one copy of the hemoglobin A gene harboring the genetic mutation found in sickle cell disease (HbS). These individuals do not have sickle cell disease but can develop kidney disease. These people may show visible (gross) hematuria (blood in the urine), abdominal or back/flank pain, abdominal mass, enlarged lymph nodes and significant weight loss.
-
Transitional cell carcinoma of the kidney, renal pelvis - Transitional cell carcinoma (TCC, more recently referred to as urothelial cell carcinoma or UCC) is a type of cancer that typically occurs in the lining of the urinary system - the kidney, bladder, and ureters). It is the most common type of bladder cancer and cancer of the ureter, urethra. It is the second most common type of kidney cancer (following renal cell carcinoma), but accounts for only five to 10 percent of all primary renal malignant tumors. Treatment is similar to that of bladder cancer and includes surgery and sometimes chemotherapy.
-
Suggested Resources: http://bladdercancercanada.org/en/
-
-
See:
Linehan WM et al, “Genetic Basis of Cancer of the Kidney: Disease-Specific Approaches to Therapy,” Clin Cancer Res September 15, 2004 10; 6282S –http://clincancerres.aacrjournals.org/content/10/18/6282S.abstract
Linehan WM et al, “Genetic basis of kidney cancer: role of genomics for the development of disease-based therapeutics.” Genome Res 2012, 22:2089-100 –http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3483538/


Add new comment